Does Medicare Cover Physical Therapy?
Read our guide to find out about Medicare coverage for physical therapy.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
Physical therapy helps people recover from injuries, eases pain, treats chronic conditions, and ultimately aims to improve the quality of life and the health of patients.
If you have mobility problems, physical limitations, or health problems keeping you from actively living your life, physical therapy may be the solution for you.
This article will cover everything you need to know about the costs of physical therapy and Medicare.
What Is Medicare?
The federal Medicare program offers health insurance to people over 65, those suffering from End-Stage Renal Disease (ESRD), and some disabled young adults.
What Are the Different Parts of Medicare?
Medicare Part A covers inpatient or hospital-related costs, services, and items.
Medicare Part B covers outpatient services, such as medically necessary and preventative services. This includes outpatient treatment, doctors' services, tests, and examinations.
Medicare Part D (prescription drug coverage) covers the cost of prescription drugs and is provided by private companies that are approved by Medicare.
You can get coverage through:
Original Medicare: This is government-run Medicare that covers Part A and Part B expenses, including some forms of physical therapy.
Medicare Supplemental Insurance: Medicare Supplement Insurance is standardized plans that offer additional coverage for inpatient and outpatient costs. For example, for foreign travel emergencies or coinsurance payments.
Medicare Advantage: These are plans offered by private insurance companies that offer coverage for Part A, Part B, and sometimes Part D costs.
What Is Physical Therapy?
Physical therapy is a non-invasive treatment used to help people develop and maintain their overall physical ability.
It helps people maintain, or regain, physical strength using fitness testing, medical checks, prognosis, and rehabilitation.

Source: Unsplash
Does Medicare Cover Physical Therapy?
Physical therapy, occupational therapy, and speech therapy are covered under Medicare.
Government-funded health insurance no longer limits the amount of coverage it will provide to cover medically essential therapeutic care.
Previously Medicare had an annual cap on payments for therapeutic services, but it was removed in 2018.
Physical therapy costs are usually included under Medicare Part B, which covers medically necessary outpatient therapy services and other outpatient procedures.
Keep in mind that Medicare checks every $3,000 spent in a calendar year to ensure that the sessions are medically necessary.

Source: Pexels
What Does Medically Necessary Mean?
Medically necessary is a definition used by Medicare to determine whether a procedure will be covered by Medicare Part A or Part B.
A medically necessary procedure is defined as services or supplies related to health care which are required to diagnose or treat a sickness, injury, condition, disease, or its symptoms.
Medically necessary services include:
Vaccinations, such as flu shots
Lab tests
X-rays
Mental health services
Be sure to ask your doctor or physical therapist how much they charge per appointment, since some of them may charge more than what Medicare covers.
Medicare will only cover your treatment up to its approved amounts, which means that you will have to cover anything above this.
For example, let’s say your physical therapist charges $250 per session but Medicare only covers $220 of the bill. You’ll have to pay $44 (20%) of the cost under Part B, and Medicare will cover $176. However, you’ll also have to pay the difference as well ($30). This means your total costs will be $74 ($44+$30).
Source: Pexels
How Can I Get Medicare to Cover My Physical Therapy?
Medicare does cover physical therapy. However, it must be approved by a registered physician and be medically necessary in order to be covered.
How do I get approval for my physical therapy?
For physical therapy to be covered through Medicare, you must have Original Medicare or a Medicare Part C plan.
You need to make sure you pay your monthly premiums and plan payments, including your Part B premium.
Physical therapy is only covered by Medicare if it is considered medically necessary.
There is no limit to how many physical therapy treatments you can have within a year, provided your doctor certifies that the treatment is necessary.
The exact amount will vary, so it's important to check whether Medicare covers your physical therapy sessions. This includes the type of treatment you receive and any other insurance coverage you may have.
For example, if a patient needs urgent physical therapy sessions because of an accident, Medicare will cover them.
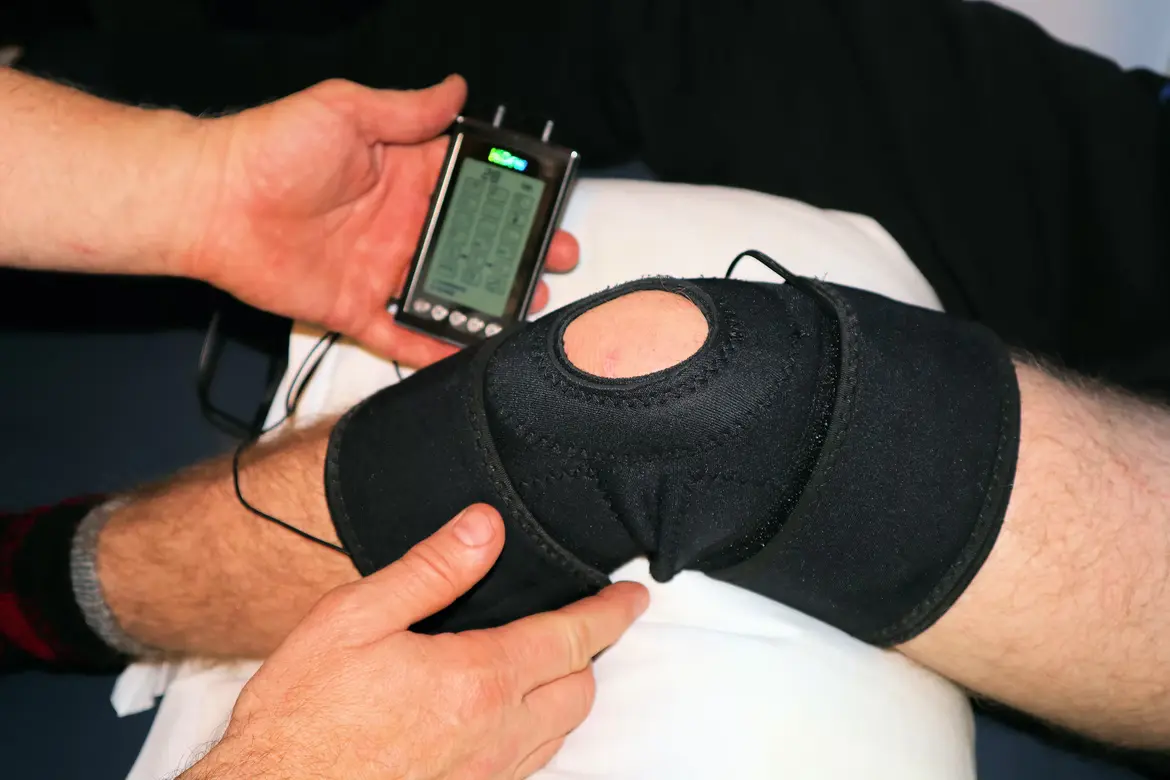
Source: Unsplash
Medicare Part A and Inpatient Physical Therapy Coverage
Your doctor might recommend inpatient rehabilitation following a serious injury like a fall or motor accident, or for a chronic condition such as Parkinson’s disease that would require ongoing physical therapy services.
These treatments will fall under Medicare Part A at inpatient rehabilitation facilities. However, you are still responsible for deductibles and coinsurance.
Here’s what you can expect to pay in 2022 if you use your Medicare Part A:
You’ll have to pay a Part A deductible ($1,556 for each benefit period) before Medicare will cover your expenses. Once you get the treatment you’ll be responsible for part of the costs, depending on how long you were in the hospital. This is known as coinsurance.
In 2022, Part A coinsurance increased slightly from the previous year.
Here’s what you’ll pay each day if you are treated in hospital and have covered your deductible.
Days 1-60: $0
Days 61-90: $389
Days 91< (Lifetime Reserve Days): $778
Terms you should know:
Deductibles: How much you have to pay for health care services before your insurer starts paying.
Coinsurance: This is the amount you have to pay for medical services, tests and items after the deductible is paid.
Benefit Periods: This is the length of time that you’ll be able to use your Medicare benefits. For Part B, the benefit period is annual. For Part A, it starts the day you are admitted and ends after 60 consecutive days of being out of hospital.
Copayments: A set fee that you have to pay after you have paid your deductible. For example, your health plan covers $100 for a doctor's visit. The copayment for the visit is $20 (80%).
Approved Amounts: Money paid by Medicare to a healthcare provider based on what is accepted as reasonable. Usually less than the actual cost.
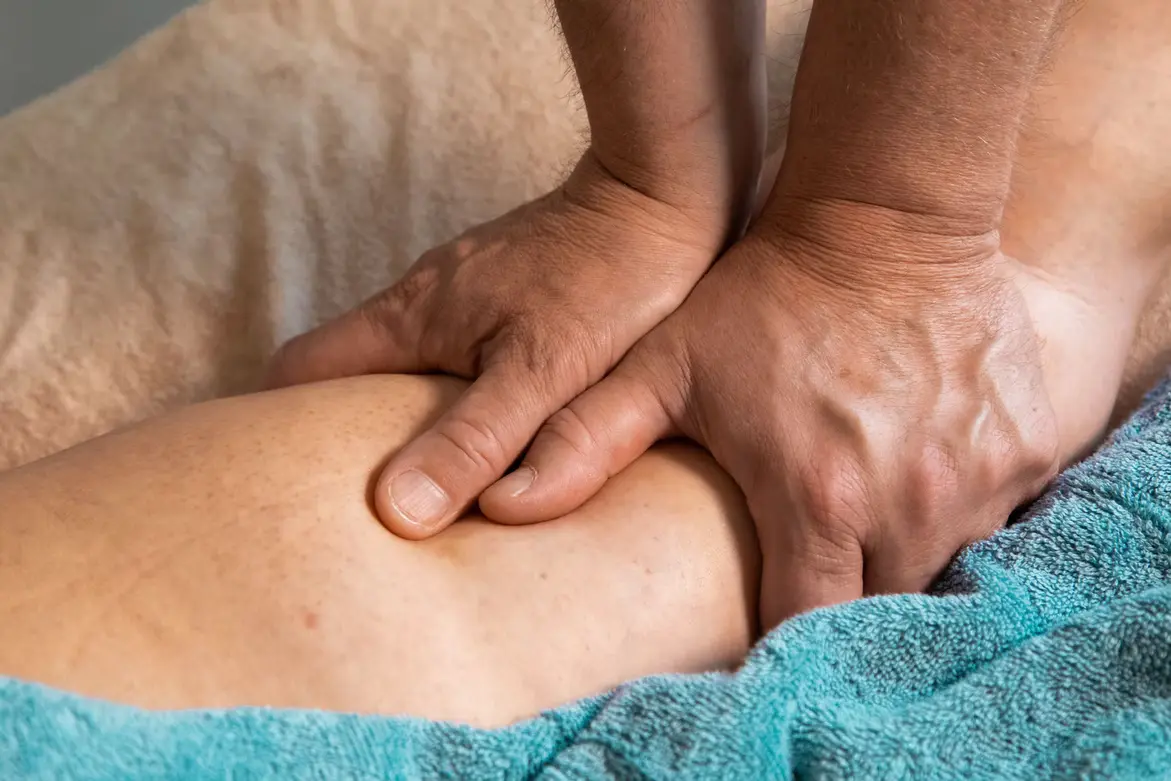
Source: Unsplash
Medicare Part B and Outpatient Physical Therapy Coverage
Outpatient physical therapy is covered by Medicare Part B by various providers including private practitioners, physical therapists, and certain in-home health care companies.
For people who qualify, there is no fee for outpatient physical therapy treatments. Part B will cover 80% of medically necessary physical therapy services. You will have to pay the remaining 20% after your deductible.
For example, if a person goes to a physical therapist that charges more than the Medicare-approved rates, they will not receive the full 80% of the costs covered.
The Medicare-approved rate will be covered, but the patient will have to pay the extra 20% along with the excess amount (up to 15% over the Medicare-approved rate).
The Medicare Eligibility Checklist for In-Home Physical Therapy
The doctor/physical therapist must be your primary doctor or examining physician
You must have a care plan created and regularly reviewed by your primary doctor
The following must be certified by your doctor/physical therapist:
On-and-off nursing/physical therapist assistance (other than drawing blood).
Physical therapy administered over a reasonable amount of time that is:
-Focused
-Safe
-Appropriate to your medical condition
-Done by a Medicare-approved provider
- You are permanently staying at home

Source: Pexels
What Can I Expect During a Physical Therapy Session?
A qualified professional normally works with patients during hour-long sessions.
Within that time they’ll walk you through exercises specific to your condition, or specific parts of your body such as your feet or hands.
Your physical therapy provider may use props to assist with daily living, such as rowing machines, during your sessions.
Exercises may also include a range of motion practices, weight-bearing activities, and strength training. Some of these will also involve props, such as light weights or balls.
Physical therapy may be beneficial for a wide range of conditions, including:
Parkinson’s disease
Alzheimer’s disease
Dementia
Multiple sclerosis
Ankylosing spondylitis
Arthritis
Hip or knee replacement
Tendonitis
Does Medicare Cover Other Types of Therapy?
Physical therapy isn't the only kind of therapy that's covered by Medicare. There are other forms of treatment that you can claim through your Medicare Part A and Part B.
These include:
Occupational therapy
Speech-language pathology
Radiation therapy
Cardiovascular behavioral therapy
Nutrition therapy
Obesity behavioral therapy
Hyperbaric oxygen therapy
Rehabilitation

Source: Pexels
Where Can I Learn More about Medicare?
If you want to learn more about Medicare enrollments, costs, and coverage, check out our Medicare Hub to learn more.
You can also look through and compare Medicare Advantage Plan quotes with our comparison tool to find a plan that offers coverage for physical therapy.
If you need more personalized assistance with your Medicare questions, call PolicyScout at 1-888-912-2132 or email help@policyscout.com to speak to a trained Medicare consultant.
Source: Pexels