Does Medicare Cover Home Health Care?
Find out everything you need to know about Medicare and its coverage for home health care.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
According to Statista, a global data analysis company, there were around 814,300 people employed as home health aides in the U.S. in 2016.
Home health care agencies can provide various services for patients depending on their conditions and medical needs.
If you are considering home health care, we can help you find the perfect policy for you.
This article will cover everything you need to know about getting Medicare coverage for home health care services.
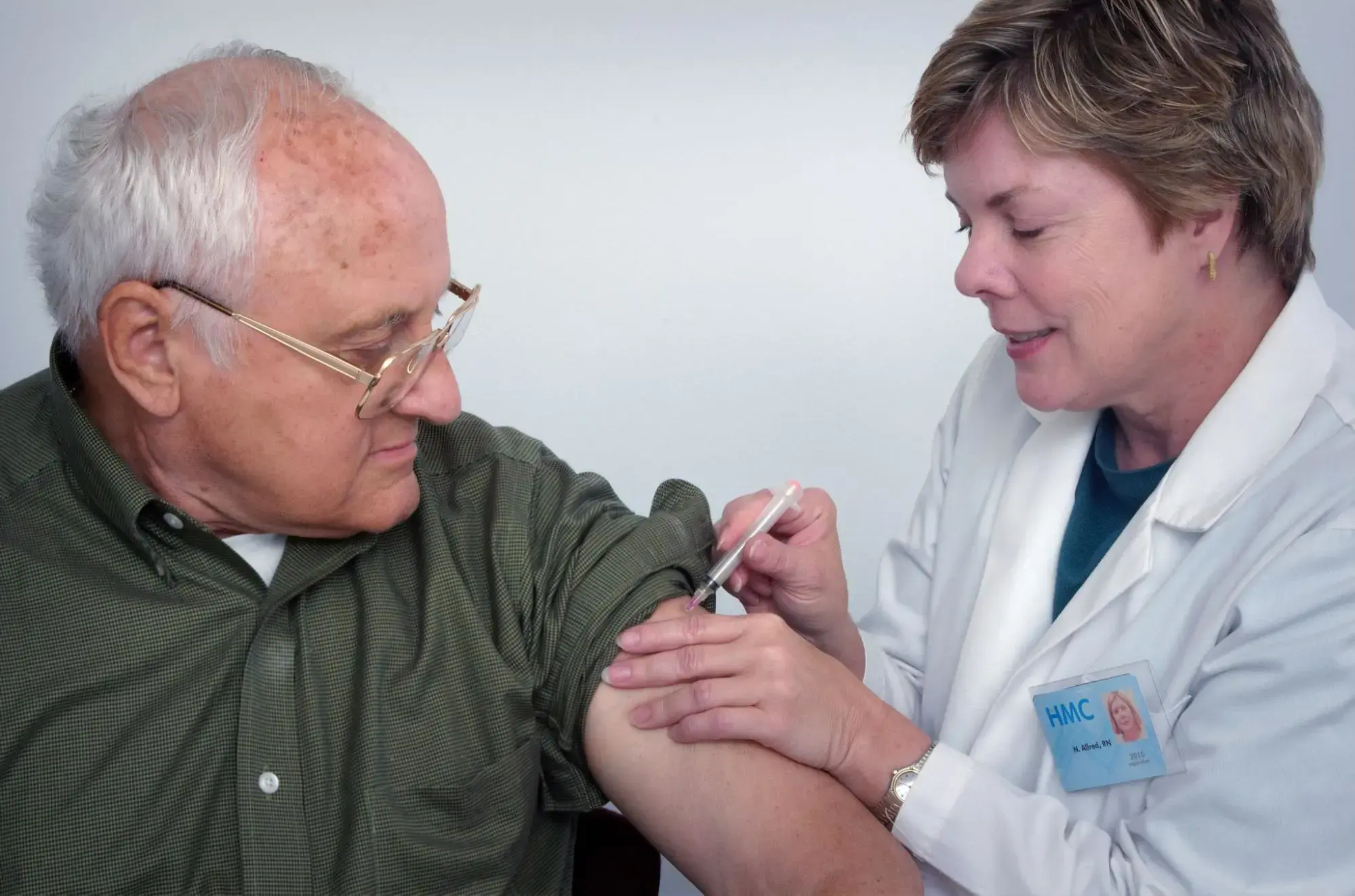
Source: Unsplash
What Is Home Health Care?
Home health care is medical care that is given to a patient at home to treat diseases or injuries.
There is a range of treatments that people can receive in the comfort of their own home, including nursing care, physical therapy, occupational therapy, and speech therapy.
People who need home health care can also get skilled non-medical care, such as medical social services, or help with daily living from a qualified home health aide.
What Is a Home Health Aide?
Home health aides provide routine personal care, such as helping elderly, recovering, or disabled persons with bathing, dressing or grooming in their own homes or in a residential care facility.
They can also assist nursing or medical staff with health-related services such as giving oral medications.
Home health care is growing in popularity because it is:
Affordable
Easy to get
Offers the same level of service as you'd get in a hospital
Medicare Coverage for Home Health Services
Which Home Health Care Services Are Covered by Medicare?
Original Medicare (Part A and Part B) covers the following services:
Part-time in-house health care aides: They provide care in a person’s own home or a residential care facility.
Part-time nursing: Slightly more medically advanced care than aides.
Occupational therapy (OT): Helps anyone with physical, sensory, or cognitive problems.
Physical therapy (PT): Helps injured or ill people improve movement and manage pain.
Women's injectable osteoporosis medicines: It helps patients treat weak and brittle bones.
Durable home medical devices and supplies: These include items such as blood sugar meters, blood sugar test strips, canes, commode chairs, hospital beds, etc.
Medical social services: Assist doctors, nurses, physical therapists, and administrative staff to care for patients.
Speech-language pathology services: The diagnosis and treatment of communication disorders.
What Is Original Medicare?
Original Medicare consists of Medicare Part A and Part B.
Medicare Part A covers inpatient care and services in hospitals, skilled nursing facilities, nursing homes, and hospices.
Medicare Part B covers outpatient services such as doctors’ visits, tests, and consultations. Part B also covers screening and preventative treatments.
What Home Health Services Does Medicare Not Cover?
Original Medicare covers a wide variety of home health care services. There are, however, a few aspects of home health care that Medicare doesn’t cover, including:
Full-time home health care
Personal care (such as dressing, bathing, or toilet assistance)
Domestic services (such as cleaning, laundry, or shopping)
Meal delivery
How to Become Eligible for In-Home Care?
There are five requirements that an individual needs to fulfill to become eligible for home health care:
1. A person applying for home health service coverage through Medicare must:
Be under the care of a doctor
Get services under a plan of care that's been set up and checked by a doctor
2. A doctor needs to confirm that you need one or more of the following:
Intermittent skilled nursing care (other than drawing blood)
Physical therapy
Speech-language pathology services
Continued occupational therapy
3. Your home health care agency needs to be Medicare-approved.
4. A doctor needs to certify that you are housebound.
What Does It Mean to Be Housebound?
A person is defined as housebound if:
They struggle to leave their house because of an illness or injury. This can mean that they rely on a cane, walker, or wheelchair, or need special assistance.
It would cause harm to them when they leave their house, because of their illness.
5. A doctor must document that they’ve met you in person and that the consultation was related to the reason you need home health care.
How Much Does Home Health Care Cost?
A 2021 survey by Genworth Financial, a Fortune 500 insurance company, found that the average cost of in-home care in the U.S. is $4,290 per month, which is about the same as the average monthly cost of a hotel room.
However, different policies cover different aspects of home health care, which means it is best to look at individual treatments and services if you’d like to find out about potential costs.
In-home care can either be very expensive or very cheap, depending on the area.
Residents of Louisiana, for example, pay an average of $3,218 a month for in-home care, which saves them over $1,000 a month compared to the national average.
It costs about $5,720 a month for the same services in Washington, which is almost $2,000 above the national average.
Because of the medical certifications and training required for caregivers, home health care is almost always more expensive than basic in-home care, no matter what state you live in.
What Are My Options to Pay for Home Health Care?
Medicare
As mentioned above, Medicare doesn't pay for standard home care, but it does pay for in-home health care, with a few limitations.
Medicare doesn't cover personal care services, like help with activities of daily living (ADL). If help with ADL, however, is all that the patient needs, it will cover these services if they are offered by a Medicare-approved provider.
What Are Activities of Daily Living (ADL)?
There are five ADLs, namely:
Bathing: This includes personal hygiene and grooming.
Dressing: This includes dressing and undressing.
Transferring: This includes movement and mobility.
Toileting: This involves continence-related tasks, including control and hygiene.
Eating: This includes preparing food and feeding.
Some Medicare Advantage Plans may also cover personal care services.
There are a lot of Medicare Advantage Plan options, so it's important to read the fine print and make sure that the plan you're interested in includes home care services as a part of the package.
What Are Medicare Advantage Plans?
Medicare Advantage, also known as Medicare Part C, covers inpatient hospital care, mental health services, rehabilitation services, and hospice care.
Private Insurance
When a person has private insurance, some of the costs of in-home care may be covered. Most long-term care services, such as home care, are not covered by standard insurance policies, only by long-term care insurance.
Long-term care insurance usually covers most aspects of in-home care for the elderly. However, coverage varies based on:
The insurance provider
The specific policy
The age of the beneficiary
When the beneficiary signed up for the policy
Medicare Advantage and Medicare Supplement Insurance for Home Health Care
All Medicare Advantage Plans must provide at least an equal level of home health care coverage to Original Medicare.
However, they may impose different rules, restrictions, and costs. Depending on your plan, you may need to:
Get care from a home health care agency that has been approved by your plan
Request a referral before receiving home health care
Pay a co-payment for care that is not fully covered
What Is a Co-Payment?
A co-payment is a predetermined rate you pay for health care services at the time of care.
For example, you may have a $25 co-payment every time you see your primary care physician, a $10 co-payment for each monthly medication, and a $250 co-payment for an emergency room visit.
You must be aware of the fact that home health care agencies are allowed to refuse to provide you with home health care services if they do not believe they can ensure your safety.
Even if no home health care agency in your plan’s network will take you as a patient, your plan must still provide you with home health care if your doctor says it is medically necessary.
For example, if no in-network home health care agency will provide you with care, but an out-of-network home health care agency will, your plan must cover your out-of-network home health care.
If you need information about the costs and coverage rules for home health care, or if you are experiencing problems, have a look at PolicyScout’s information on Medicare Advantage Plans.
Where Can I Learn More about Medicare?
Getting older often requires specific types of medical care, one of which is home health care services.
We know that choosing Medicare coverage that meets your needs can be tricky. At PolicyScout, we have many resources to make this decision easier.
Check out our Medicare hub to learn about Medicare and how to find the right cover.
You can also reach out to one of our trained consultants at 1-888-912-2132 or at help@policyscout.com to get advice and guidance on providers and plans in your area.