What Is Durable Medical Equipment (And Will Medicare Cover It?)
Find out what Medicare classifies as durable medical equipment and what you can get covered.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
If you have a chronic health condition that requires medical devices or equipment, you might be able to get the costs covered by Medicare. Medicare Part B covers some types of durable medical equipment (DME), but many people don’t know which costs they can claim back.
This article will help you understand what durable medical equipment is, what types of DME Medicare Part B covers, and what you should know about claiming equipment costs back.
What Is Durable Medical Equipment?
Medicare defines durable medical equipment as any device that:
Is used primarily for a medical purpose
Can be used over and over again
Must be used at home
Must have an expected lifetime of at least three years
Can only be helpful to patients with an injury, disability, or chronic condition
You will also have to get a recommendation from your referring doctor if you want your medical equipment to be covered by Medicare.
However, there are some exceptions to these general rules.
For example, blood sugar test strips can only be used once. However, they are considered to be durable medical equipment and are covered by Medicare.
What Does Medicare Consider to be Durable Medical Equipment?
Some common examples of durable medical equipment include:
Personal care aids like bath chairs, dressing aids, and commodes
Mobility aids such as walkers, crutches, wheelchairs, and scooters
Bed equipment and hospital beds
Home dialysis machines
Traction equipment
Prostheses
Oxygen concentrators
Oxygen monitors
Ventilators
Which Part of Medicare Covers Durable Medical Equipment?
If you want your durable medical equipment covered by Medicare, you can do this through your Part B cover.
If you have Medicare Advantage, you’ll need to submit claims through your health insurance company.
What Is Medicare?
Medicare is a health scheme operated by the United States government for people over the age of 65 and people of any age who suffer from ESRD (End-Stage Renal Disease) and ALS (Amyotrophic Lateral Sclerosis).
The scheme is divided into three parts (A, B, and D) which cover different types of expenses.
Whether you have federal government Medicare or Medicare Advantage, you will be covered for the exact same amount.
This is because the Centers for Medicare and Medicaid Services (CMS) require that all Medicare Advantage providers offer the same level of coverage as Original Medicare does.

Source: Pexels
What Is Medicare Part B?
Medicare Part B covers outpatient or non-hospital medical expenses. Joining Medicare Part B is optional, and you’ll need to pay a monthly premium to get it.
The amount you pay each month will depend on when you join Medicare Part B and your annual income tax return in the previous year.
The standard monthly rate was $148.50 in 2021, and in 2022 it has increased to $170.10.
There’s also an annual deductible with Medicare Part B. In 2021 this was $203, and in 2022 it is $233.
How Do I Sign Up for Medicare Part B?
If you haven’t joined Medicare Part B, you can contact the Centers for Medicare and Medicaid Services (CMS), who will assist you.
If you have a Medicare Advantage plan, you’re probably already signed up for Medicare Part B.
This is because when you join Medicare through a Medicare Advantage plan, your provider covers Part A, Part B, and sometimes Part D expenses.
Keep in mind that there is a late joiner’s penalty if you sign up for Medicare Part B after your 65th birthday.
This penalty is based on the number of 12-month periods that you weren’t enrolled in Part B. Medicare charges a 10% increase on the standard premium rate for each 12-month period that a person didn’t join after they’ve turned 65.
For example, if you became eligible for Medicare Part B in 2019 but only joined 24 months later, you would have to pay 20% more each month.
This means that instead of paying the $170.10 standard Part B premium, you’d have to pay $204.12 (20% more).

Source: Pexels
How Do I Get Durable Medical Equipment Covered by Medicare?
Medicare Part B will only cover durable medical equipment for home use. This means that if you are in hospital, you won’t be covered for durable medical equipment, and the cost will fall under your Part A expenses.
If you are a resident of a long-term care facility or a hospice, you may have to file additional paperwork to get covered.
However, these facilities can be considered your home if you are a long-term resident, allowing you to claim from Medicare Part B.
If you are admitted to a hospital, skilled nurse facility, or nursing home, these facilities are not considered your home.
Skilled Nursing Facilities and Durable Medical Equipment
A skilled nursing facility is required to provide you with all the durable medical equipment you need for the first 100 days of treatment.
This includes equipment, such as:
Oxygen Equipment
Hospital Beds
If this is not the case, our advice is to reach out to the Centers for Medicare and Medicaid Services to find out how to get equipment that is a medical necessity.
Steps you will need to take to get your durable medical equipment covered under Medicare Part B:
Firstly, ask your referring physician to write a recommendation for the equipment you’ll need to manage your condition.
Secondly, make sure that your condition makes the prescribed treatment, device, or test medically necessary.
Medicare will only cover medically necessary, durable medical equipment if you have been formally diagnosed with a condition, such as diabetes, cardiovascular disease, or sleep apnea.
Source: Pexels
What Does Medically Necessary Mean?
Medically necessary is a measure that Medicare uses to decide whether or not to cover medical costs.
In order for treatments, devices, or screenings to be categorized as medically necessary, it must be:
1) Recommended by a registered medical professional
2) Treat, diagnose, or relieve the symptoms of an illness, injury, or disease
If you’d like to learn more about getting coverage for medically necessary services, reach out to our Medicare agents on 1-888-912-2132.
Thirdly, visit the federal government website Supplier Directory and search for a medical equipment supplier in your area.
If you can’t find a supplier in your area, search for one online using Google, or see if suppliers will ship the device or equipment to your address.
If you have a Medicare Advantage plan, speak to your health provider and ask them what you must do to get your medically necessary durable equipment covered by your health plan.
Remember, Medicare Advantage plans must provide the same level of cover as Original Medicare.
Durable Medical Equipment for Diabetics
If you have diabetes, you’ll have to follow the same procedure we’ve covered above and get a recommendation for the device or item you need.
There are several items and devices that the CMS include on their list of durable medical equipment.
This includes diabetes self-testing equipment, such as:
Insulin Needles
Infusion pumps and supplies
Lancet devices and lancets
Blood sugar meters
Blood sugar test strips
However, it’s important to remember that Medicare will not pay for all devices and equipment, so always check with your doctor or primary caregiver before making a purchase.
Medicare and Durable Medical Equipment for Diabetes
Keep these points in mind for diabetic durable medical equipment:
Some devices, such as an artificial pancreas device system, are only covered by Medicare if you are admitted as a patient.
This means that you won’t be able to claim back the cost of this device if you aren’t receiving treatment in a hospital under Medicare Part A.
A person with diabetes can get one pair of custom-molded shoes covered by Medicare per calendar year.
Other equipment, such as an infusion pump system, are not covered by Medicare.
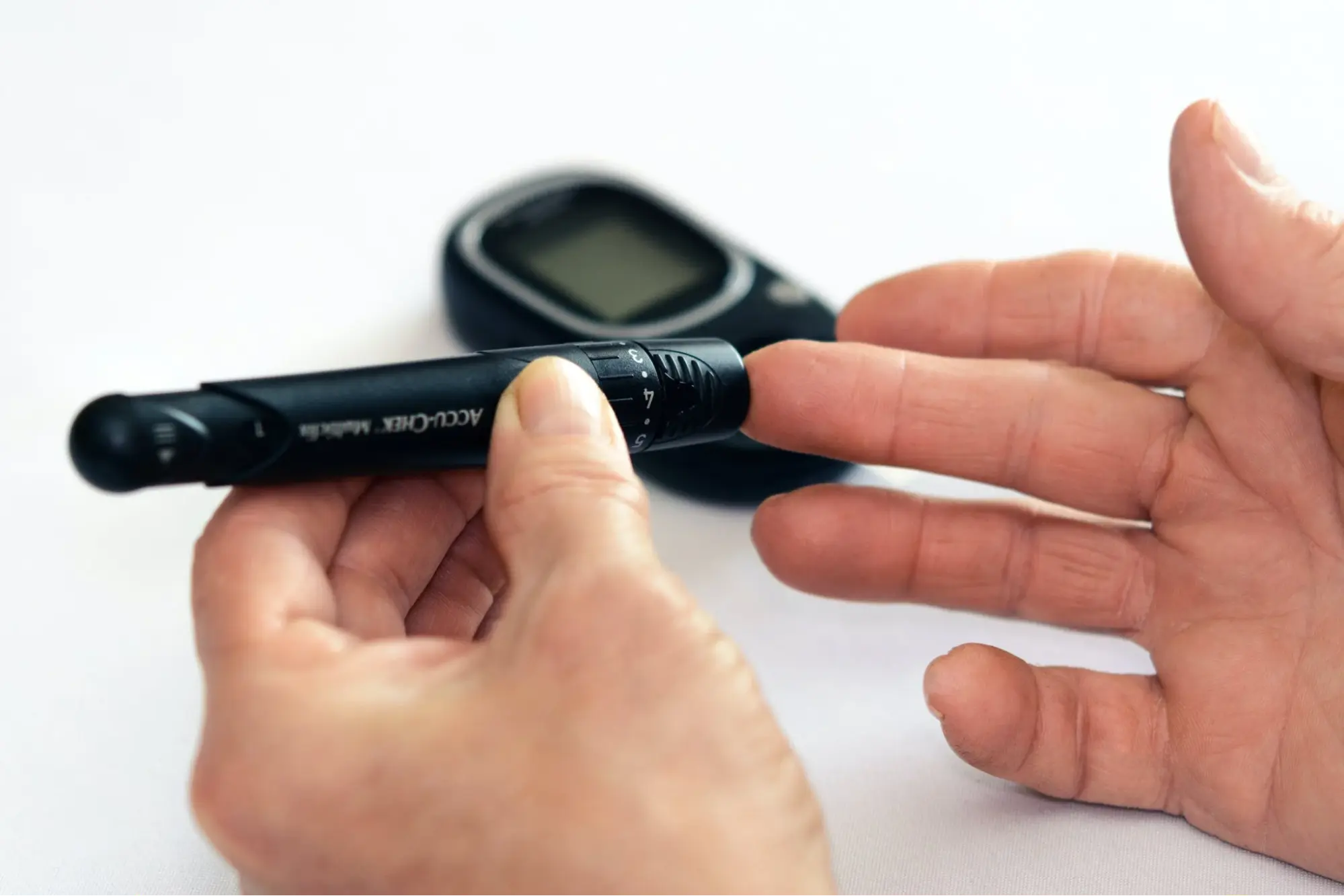
Source: Pexels
Durable Medicare Equipment for Cardiovascular Diseases
People with cardiovascular diseases such as high blood pressure, cholesterol, arterial sclerosis, as well as sleep apnea, can apply to get their durable medical equipment covered by Medicare.
Some common examples of items covered by the CMS include:
A CPAP machine
Oxygen Equipment
The costs of these devices are covered under your Medicare Part B, which means that the CMS will pay 80% of the price and you will have to cover 20%.
For example, if your CPAP machine costs $500, Medicare Part B will cover $400 (80% of the cost). You will need to pay 20% ($100).
Durable Medical Equipment and Vision Care
Medicare will cover some types of durable medical equipment for vision care. However, they do not cover eyeglasses.
If you undergo cataract surgery with Medicare Plan B, Medicare will cover 80% of the cost of corrective lenses. You will have to pay 20% of the costs.
If you would like to get more comprehensive cover for glasses and other types of durable medical equipment for vision, Medicare Advantage plans might be the right option for you.
These private plans offer additional coverage for vision, dental, and hearing expenses.
In some cases, your Medicare Advantage plan might cover the total cost of getting eyeglasses if you use a network provider.
What Is a Network Provider?
A network provider is a healthcare professional contracted into your Medicare Advantage plan.
Depending on your plan, your health insurance may only cover some of the costs of seeing a provider that is not in their network, or out-of-network.
Our advice is to check with your doctor, specialist, or health professional if your plan covers them before you go see them.
You can also reach out to your Medicare Advantage insurance plan providers and ask them for a list of approved health care providers that form part of their network.

Source: Pexels
Durable Medical Equipment Coverage for Prosthetic Devices
As long as the device is ordered by a medical professional and for a medical purpose, Medicare will cover any prosthetic device that replaces a body part or function.
Medicare will also cover some types of prosthetic devices, including:
Prosthetic limbs
Ostomy Bags
Some types of surgically implanted prosthetic devices
Eyeglasses and corrective lenses
Remember that Medicare pays 80% of the Medicare-approved amount. If your device or prosthetic is more expensive, then Medicare will not cover the entire cost.
What Does Assignment Mean?
An assignment is a Medicare-approved amount for an item, test, or service. For example, if a doctor accepts assignment for their services, this means they will accept the Medicare rate.
Other Options for Paying for Durable Medical Equipment
As we’ve mentioned already, Medicare Advantage plans usually offer additional coverage and benefits.
If you are concerned about the ongoing costs of your durable medical equipment, try finding a Medicare Advantage provider that offers specific coverage for your condition.
Another option is to get Medicare Supplement Insurance, which helps to pay for additional Medicare costs such as deductibles, coinsurance, and extended hospital stays.
If you’d like to find out more about these plans, reach out to our consultants to find a plan that will cover your chronic medical needs so that you can keep up with your durable medical equipment costs.
Where Can I Learn More about Medicare?
If you’re new to Medicare or want to know more about Medicare Advantage, Medicare Supplement Insurance, or Part D plans, our Medicare hub is a great place to start.
We have articles on coverage, enrollment, costs, penalties, as well as other topics that will help you navigate through Medicare.
As always, if you need help with a specific question, reach out to one of our Medicare agents at 1-888-912-2132 or send an email to help@policyscout.com for assistance. We are here to help you get the best Medicare coverage you possibly can.