Does Medicare Cover Dermatology?
Dermatology is a large field that treats many issues: some of which are covered by Medicare. Find out if what you need is covered here.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
Dermatology deals with various skin, hair, and nail disorders. You might want to visit a dermatologist for reasons as wide-ranging as cancer, acne, cosmetic procedures, hair and nail issues, and more.
Medicare coverage helps with many of these issues, but not all of them. Avoid unexpected expenses by confirming that the reason for your visit is covered before you make a trip.
Key Takeaways:
Medicare plans cover dermatological treatments that are medically necessary.
It covers checks for specific issues, but not general screenings.
You may still have out-of-pocket costs, including your deductible and coinsurance.

(Source: Pexels)
Does Original Medicare Cover Dermatology?
The simple answer is that it depends on what you want to see a dermatologist for.
Original Medicare (Parts A and Part B) covers consultations and treatment if the problem is medically necessary. Medically necessary treatments include some chronic skin issues and cancer.
Medicare Part A vs. Part B
| Part A | Part B |
|---|---|
| Part A covers inpatient care in medical facilities such as hospitals. It will cover you if you are admitted to hospital due to a skin issue. For example, if you need surgery to remove a melanoma. | Part B covers outpatient care. This includes medically necessary services and preventative services. It will cover you when you receive medically necessary outpatient dermatology services. For example, a screening for a specific issue. |
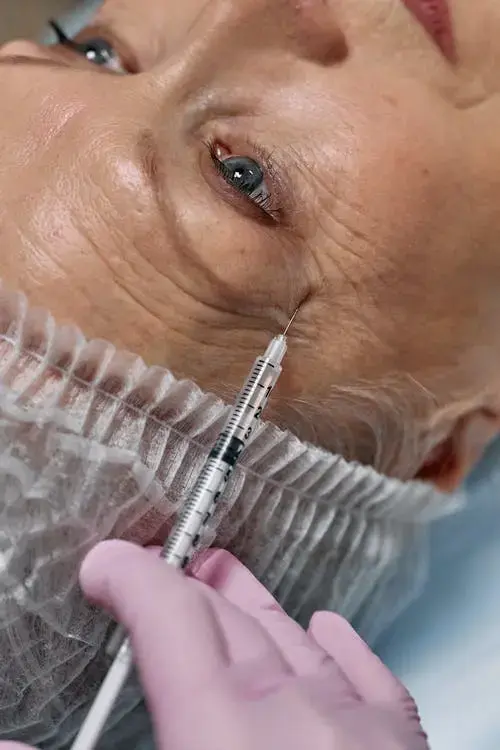
(Source: Pexels)
Medicare does not cover dermatology services that are purely cosmetic procedures. Anti-aging skin treatments, laser hair removal, and acne treatments are not typically covered.
But Medicare may cover treatments that are often considered cosmetic if the treatment has a medical purpose.
Treatments Original Medicare Might Cover
Excess skin removal after weight loss may be covered if the skin is causing pain or discomfort.
Botox injections to treat muscle disorders.
Rhinoplasty surgery after an injury.
You must get prior authorization from Medicare before undergoing one of these procedures. Your health care provider will take care of the approval application process.
The visit to your dermatologist must also be for a specific medical treatment for Medicare to cover it. It will cover you if you want to get a specific mole checked, for example, but it will not cover a full-body skin exam.
Drugs related to your skin condition might be covered by Medicare. Original Medicare offers some coverage—typically for drugs, you receive in a hospital or outpatient setting. You can get coverage for prescription drugs by taking out a Medicare Part D plan or switching to a Medicare Advantage plan with prescription drug coverage.
How about Medicare Advantage Plans?
Part C Plans (Medicare Advantage) are private insurance policies that follow the rules set by Medicare. They all offer Medicare Part A and Part B coverage and usually include some form of prescription drug coverage (Part D).
If you have a Part C plan it means your plan may pay for dermatological services that aren’t covered under Part A and Part B. This could include drugs that aren’t covered under original Medicare and routine screenings.
However, plan coverage varies depending on your location and insurance provider. If you have a Medicare Advantage (Part C) plan, contact your insurance provider to discover if it offers the additional treatment you need.
Medicare Advantage plans may require you to use health care providers in your plan’s network. Contact your insurance company before visiting a dermatologist to find an in-network provider.
Does Original Medicare Cover Skin Cancer Screening and Treatment?
Skin cancer screenings are covered under Medicare in some circumstances. It will cover visits to your doctor if you notice a mole or skin growth that you are worried about. But it will not usually cover screenings if you aren’t symptomatic.
Original Medicare will provide further help to treat skin cancer if you need it. Medicare Part A (hospital insurance) covers hospital stays, surgery, blood work, and other related treatment. Part B (medical insurance) covers outpatient treatment and care such as radiation tests and X-rays.
What Is the Cost of Dermatology with Medicare?
The amount you pay depends on multiple factors, including whether the treatment falls under Medicare Part A or B.
Medicare Part B covers medically necessary dermatology costs. It pays for 80% of the costs of relevant procedures once you’ve met your deductible. You pay the remaining 20% of the Medicare-approved amount, which means you’ll still have some out-of-pocket costs even if your treatment is covered.
Further treatment, including hospital stays, may be covered by Medicare Part A. You’ll have to pay your deductible of $1,556 per coverage period. If you stay for longer than 60 days, there is a coinsurance amount of $389 per day.
| Key term: Deductible | Key term: Coinsurance |
|---|---|
| Your deductible is the amount you must pay before Medicare will start to cover your treatment. | Coinsurance is the amount you must pay for medical treatment covered by Medicare. You must pay it even if you have met your deductible. |
| The deductible for Part B in 2022 is $233. The deductible for Medicare Part A is $1,556 per coverage period. | Coinsurance for Medicare Part B is 20% of the treatment’s Medicare-approved amount. |
| Coinsurance for Part A kicks in once you have been hospitalized for 60 days. It is $389 per day from day 61 to day 90 and $778 per lifetime reserve day after 90 days. After this, you pay full costs. |
The amount you pay for dermatology services with Medicare depends on:
The type of treatment.
The cost of your treatment.
How much of your deductible you have paid.
Your copay amount.
Whether you need additional medications.
Medicare Supplement Insurance plans can reduce the expense of dermatology treatment. They do this by helping with out-of-pocket expenses such as your deductible and coinsurance.
If you have one of these plans, contact your provider to find out more about what is and isn’t covered.

(Source: Pexels)
Do I Need a Referral to See a Dermatologist with Medicare?
You don’t typically need a referral from your primary care physician to see a dermatologist with Medicare if the visit is for a specific issue. But you should check that the treatment you are visiting for is covered before you make a trip.
You should also check that the dermatologist you want to visit accepts Medicare patients. You can do this by using the tool on the Medicare website or by contacting dermatologists in your area.
If you have a Medicare Part C plan, you will likely have to use a dermatologist in your plan’s network. You may also need a referral from your primary care doctor.
Specific, Medically Necessary Issues Are Usually Covered
Whether Medicare covers your skin issue depends on what the condition is. If it is a specific issue and treatment is considered medically necessary, there’s a good chance that you are covered. If not, you may have to pay your expenses out of pocket.
And even if your dermatology services are covered by Medicare, you will still have to pay a copay amount. Depending on other treatment you have received in the period, you may also need to pay a contribution towards your deductible.
Are you looking for help choosing a Medicare or Medicare Supplement Plan? PolicyScout can help. Find out more about how we can help you find top-rated health insurance companies and affordable Medicare plans in your area.

(Source: Pexels)