What Are Medicare Advantage HMO Plans?
Everything you need to know about Medicare Advantage HMO Plans and their implications for you.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
Health Maintenance Organizations (HMOs) are one of the six kinds of private health care plans that Medicare beneficiaries can join.
HMO Plans are ideal for some people because they offer excellent health care services at an affordable rate.
In this article, we will discuss Medicare Advantage HMO Plans, how they work, how much they cost, and why they are a good option for some people.

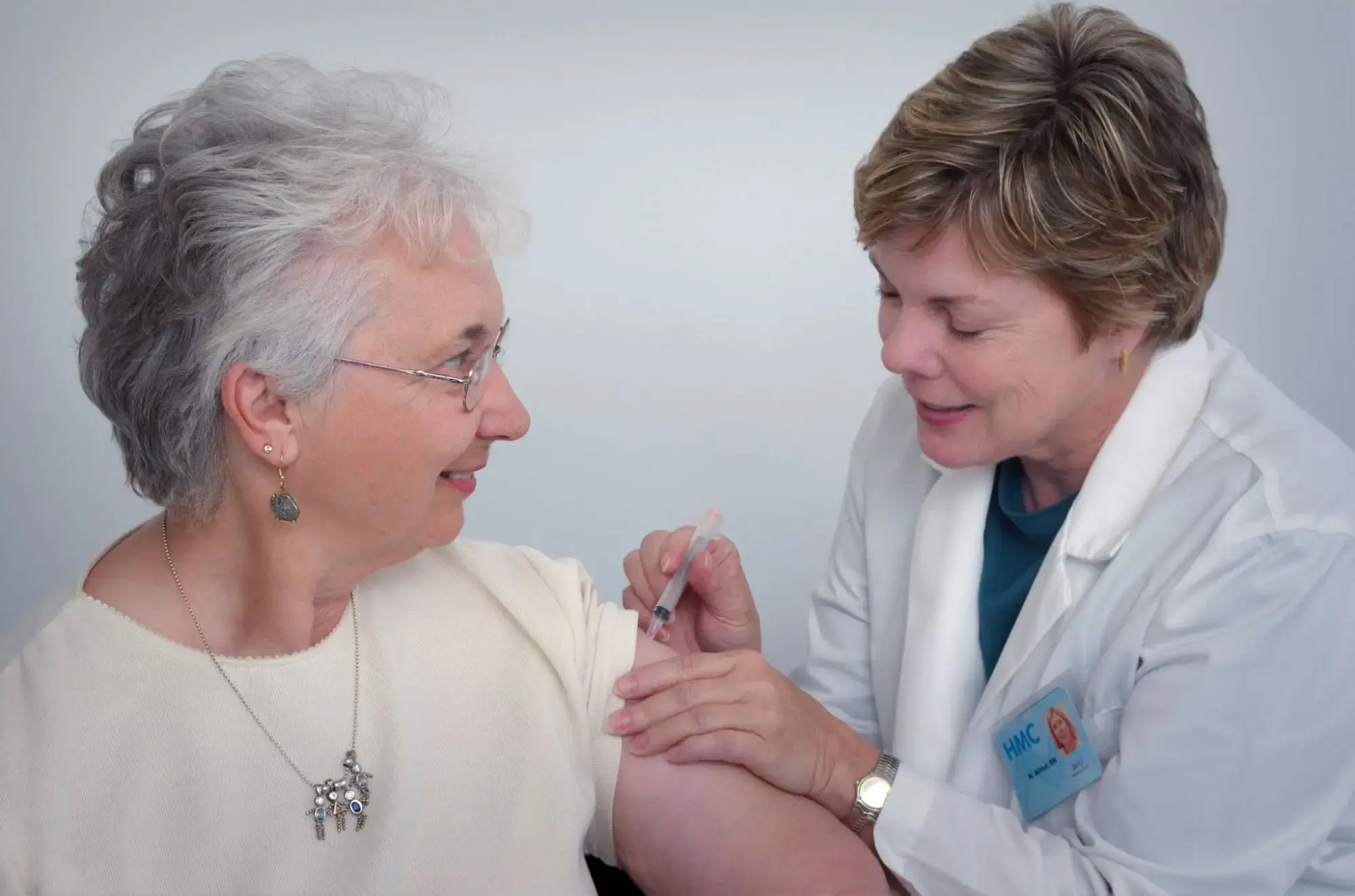
Source: Unsplash
What Is a Medicare Advantage Health Maintenance Organization (HMO) Plan?
A Health Maintenance Organization (HMO) Plan is a type of Medicare Advantage Plan that pays for certain health care services from doctors, other healthcare providers, or hospitals in the Plan's network.
What Is Medicare Advantage?
Medicare Advantage, also known as Medicare Part C, is health coverage offered by private health insurance companies.
These plans provide the same benefits as Original Medicare (Parts A and B) and additional insurance for dental, hearing, and vision expenses. Some plans also offer coverage for prescription drugs.
Some features of an HMO plan include:
A small group of providers to choose from
Less paperwork than other types of insurance plans
You need to get permission from your doctor to see a specialist
However, Medicare HMO Plans don't generally cover:
Emergency care
Out-of-area urgent care
Out-of-area dialysis
What Is Dialysis?
Dialysis is a treatment that does some of the things done by healthy kidneys. It is needed when your own kidneys can no longer take care of your body's needs.
HMO Plans also only offer coverage within set provider networks. These networks are generally local.
How Do Medicare HMO Plans Work?
Medicare Advantage HMOs are based on in-network medical care. When you need medical help, you will have to choose from a list of providers who are contracted into a provider’s network.
If you choose to go with a provider who is not in your insurance network, your provider may only cover some of the costs, or they might not cover you at all.
When you sign up for your plan, you will be given a list of in-network providers and rules about out-of-network care.
There are some types of Medicare Advantage HMOs that allow you to get services from providers who aren't in your plan’s network. These are called Point-of-Service (POS) plans, and usually have different rules than regular HMOs.
What Is a Point-of-Service (POS) Plan?
A point-of-service (POS) plan is a type of managed care plan that is a hybrid of HMO and Preferred Provider Organization (PPO) Plans.
Like an HMO, participants designate an in-network physician to be their primary care provider. But like a PPO, patients may also go outside of the provider network for health care services.

Source: Pexels
What Is an HMO with a Point-of-Service Option?
An HMO-POS Plan is an HMO Plan with extra POS benefits. This gives you more options when you need medical help. With an HMO-POS you can go outside of the network for care, but you'll pay more.
The following also applies to an HMO-POS Plan:
You'll need to pick a primary care physician (PCP) who will be in charge of all of your care.
You don't usually need a referral to see a specialist. However, your doctor may be able to help you see a specialist more quickly.
You need to get permission from your doctor for some services beforehand. If you don't, some services may not be paid for.
For the HMO and POS parts of the plan, there are two different deductibles. The two deductibles can't be combined, but rather have to be reached one at a time.
Who Is Eligible for HMO Plans?
To be eligible for an HMO Plan, a person must be enrolled in Original Medicare and live in the Plan’s service area.
What Is Original Medicare?
Original Medicare consists of Medicare Part A and Part B.
Medicare Part A covers inpatient care and services in hospitals, skilled nursing facilities, nursing homes, and hospices.
Medicare Part B covers outpatient services such as doctors’ visits, tests, and consultations. Part B also covers screening and preventative treatments.
Previously, there were other eligibility requirements for people with end-stage renal disease (ESRD), also called end-stage kidney disease or kidney failure.
However, changes in the regulations in 2021 mean that any person with ESRD can enroll in a Medicare Advantage Plan.

Source: Pexels
Pros and Cons of HMO Plans
Medicare Advantage Plans may provide more affordable coverage than you would receive otherwise. However, you have to follow the Medicare Advantage Plan’s rules to receive payment for covered services.
Let’s take a look at some of the benefits and drawbacks of a Medicare Advantage HMO Plan:
Pros of HMO Plans
These plans are a popular choice among Medicare Advantage Plans, which come with some benefits, such as:
A variety of available options
Low-cost premiums, deductibles, and co-payments in most major cities
A wide in-network selection of providers to choose from
Cons of HMO Plans
Even though these plans are popular, they come with some disadvantages, such as:
Full coverage is limited to a select network of doctors, specialists, and facilities
You may have to switch doctors if your current physician isn't on your health care provider's network
How Does an HMO Plan Differ from a PPO Plan?
A Preferred Provider Organization (PPO) Plan is a type of health plan that contracts with medical providers, such as hospitals and doctors, to create a network of participating providers.
This means you will pay less if you use providers that belong to the Plan's network.
The differences between HMO and PPO health care plans
| HMO | PPO |
|---|---|
| Lower premiums and deductibles | Higher premiums and deductibles |
| Only cover in-network services | Can go out-of-network |
| Need a referral for specialists | No need for referrals |
| No need to file claims | May need to file claims |
| Ideal for: people who want lower healthcare costs | Ideal for: people who want more control over their health care |
What Do Medicare Advantage HMO Plans Cost?
For some people, joining a Medicare Advantage HMO Plan might help them save money on health care costs.
A lot of HMO Plans don’t charge their members for services and tests that are done in-network. This means they won’t have to pay the 20% Part B coinsurance amount each time they visit the doctor. Here are some costs to think about when you choose your plan:
| Costs | Considerations |
|---|---|
| Premiums | Medicare Advantage HMOs may have their own monthly premium, unless they are zero-premium plans. However, your HMO Plan doesn’t cover the Medicare Part B premium ($170.10 per month), so you’ll pay this amount in addition to any premium that comes with your HMO Plan. |
| Deductibles | A Medicare Advantage HMO Plan generally has its own in-network deductible amounts, which can start from as low as $0. If your plan offers prescription drug coverage, you can also expect to see a prescription drug coverage deductible amount. |
| Co-payment | When you enroll in an HMO Plan, there are different co-payment amounts for primary care physician and specialist visits. Co-payments can range from $0 to $50 per visit, depending on the plan and provider. |
| Coinsurance | After the yearly plan deductible has been met, you’ll usually pay 20% of the Medicare-approved costs for the services you receive. |
| Out-of-pocket maximums | All Medicare Advantage HMO Plans have an out-of-pocket max, which varies based on the details of your plan. |
When Can I Enroll in an HMO Plan?
People can sign up for Medicare Advantage Plans, including HMO Plans, at different times throughout the year. Here are some important dates to remember:
The Initial Enrollment Period (IEP): This is the three months before and after your 65th birthday (it also includes the birthday month). For example, if your birthday is 6 June you can enroll from 1 March until 30 September of that year.
The General Enrollment Period (GEP): This is from 1 January to 31 March every year. During the GEP, you will be able to sign up for Medicare Part A and B, and join Medicare Advantage Plans.
The Open Enrollment Period (OEP): During OEP which runs from 15 October to 7 December, you'll be able to join, switch, or drop an Advantage Plan, including a Medicare HMO.
If you would like to read more about enrollment periods, check out this article about what you need to know about Medicare Open Enrollment.

Source: Pexels
Where Can I Learn More about Insurance?
A Medicare Advantage Health Maintenance Organization (HMO) Plan can be a great cost-saving opportunity because they offer low or no coinsurance for in-network services.
If you’re wondering about Medicare Advantage Plans or want to learn about the different Medicare HMO options available to you, get in touch with one of our professional consultants. Send us an email at help@policyscout.com or give us a call at 1-888-912-2132.
For more information, insurance quotes, and to get the process started, visit PolicyScout today.
Source: Unsplash