Does Medicare Cover Preexisting Conditions?
Original Medicare and Medicare Advantage Plans cover preexisting conditions. Read on to find out more.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
What Is a Preexisting Condition?
A preexisting condition is a health problem or disease you had before the start of your health care coverage. This can include disease and chronic conditions such as diabetes, high blood pressure, depression, and End-Stage Renal Disease (ESRD).
Key Takeaways:
Medicare covers preexisting conditions at no extra cost.
You can join Medicare Advantage Plans with a preexisting condition.
Medigap plans must cover your condition when bought in certain circumstances.
People with preexisting conditions often worry they won’t qualify for Medicare and Medicare Advantage cover.
But that’s not the case: your current state of health or medical history won’t affect whether or not you qualify.
If you’re enrolled for Part B cover, you are also guaranteed to be accepted for additional coverage via a Medigap plan if you are applying for the first time during the Open Enrollment Period (six months after your enrollment). However, you must apply for this coverage at the correct time.
Does Original Medicare Cover Preexisting Conditions?
Yes, Original Medicare covers preexisting conditions. There are no additional costs associated with Medicare Part A or Medicare Part B for health problems you suffer from before signing up.
Medicare Part D is an optional plan that provides more comprehensive drug coverage. This plan also covers preexisting conditions, and the amount you pay for coverage is the same as anyone else.
| Original Medicare | Additional coverage | |
|---|---|---|
| Medicare Part A (Hospital Insurance) | Medicare Part B (Medical Care) | Medicare Part D (Prescriptions Drug Coverage) |
| Covers inpatient care in a hospital, nursing home, hospice, skilled nursing facility, and some health care. | Covers medically necessary services and preventative services. | Helps cover the cost of prescription drugs. |
What about Medicare Advantage Plans?
Medicare Advantage (Part C) Plans are offered by private companies. They have the same coverage as Original Medicare, while typically offering extra benefits. This may include prescription drugs, dental, vision, and hearing coverage.
You can join one of these medical insurance plans even if you have preexisting conditions. The price of the plan depends on factors such as the provider, the plan type, and the level of coverage.
However, the price you pay will be the same as someone without a preexisting condition.
Do Medicare Supplement Insurance Plans (Medigap) Cover Preexisting Conditions?
Medicare Supplement Insurance plans (Medigap) are private Medicare policies that cover some of Medicare’s out-of-pocket costs. Each plan differs, but they can help with your out-of-pocket costs such as coinsurance and deductibles.
These plans must cover preexisting conditions if you sign up for them during your Medigap Open Enrollment Period, or if you have a guaranteed rights issue.
1. Medicare Open Enrollment Period
Medicare Open Enrollment is the six-month period that starts the first month you have a Medicare Part B plan, and you’re 65 or over.
During this time, you can buy any Medicare Supplement Insurance plan for the same price as someone without existing conditions. There is no medical underwriting process during signup at this time. This means providers won’t look at your health history.
2. Guaranteed Issue Rights
Private health insurance companies must also offer you a Medicare Supplement Insurance when you have guaranteed issue rights. This is commonly the case when a current plan is ending, or if your insurance coverage ends through no fault of your own.
What Is Medical Underwriting?
Medical underwriting is an evaluation process performed by health insurance companies. They will look at your medical history and determine:
Whether they can offer you health coverage.
What your premiums will be.
If you will have any medical exclusions.
When Can Medigap Providers Refuse to Cover Me?
A Medigap insurance company can turn down your application if you don’t meet the above criteria. Even if you do get accepted, you may end up paying more.
Medigap providers can also refuse to cover your expenses for the first six months of your coverage in some cases.
This can occur when either:
Your condition was diagnosed in the six months before the start of your Medigap policy.
You received treatment in the six months before the start of your Medigap policy.
You can avoid or shorten the preexisting condition waiting period if:
You have at least six months of existing creditable coverage
The coverage break is under 63 days.
Speak to your provider to see if your current policy counts as creditable coverage. If you’re unsure about how you can avoid Medigap policy waiting times, reach out to PolicyScout to get your questions answered.
Switching Medicare Supplement Plans with Preexisting Conditions
You may decide to switch Medigap plans if you have changing needs or think you can get a better deal.
If you decide to change Medicare Supplement Insurance plans, there is no guarantee that insurance companies will accept your application outside of the Open Enrollment Period if you don’t have guaranteed issue rights.
This means you may not be accepted for a new Medicare Supplement Plan, or it may cost more than your existing one.
If you want to switch plans, it’s best not to cancel your previous coverage until your new coverage goes into effect. You can keep your old plan for 30 days while deciding whether you are happy with your new one.
| Free Look Period |
|---|
| This is a 30-day period that begins when you start your new Medigap policy. It lets you keep your existing plan while trying out your new one. You’ll have to pay a premium for both approaches during this time, but this extra cost may be worth it for peace of mind. Once you cancel your existing coverage, you can’t get it back. |
Switching from a Medicare Advantage Plan to Medigap Coverage with a Preexisting Condition
You can switch from a Medicare Advantage Plan to a Medigap plan with preexisting conditions if an insurance company that offers Medigap accepts your application.
Alternatively, you are guaranteed coverage if you have a “trial right” to buy a policy.
This occurs when:
You are eligible for Medicare and join a Medicare Advantage Plan at 65, then decide to switch to Original Medicare within the first year.
You switch from Medigap to Medicare Advantage and within a year decide to switch back. You only have trial rights the first time you switch.
The number of people suffering from preexisting and chronic health conditions is more than people think.
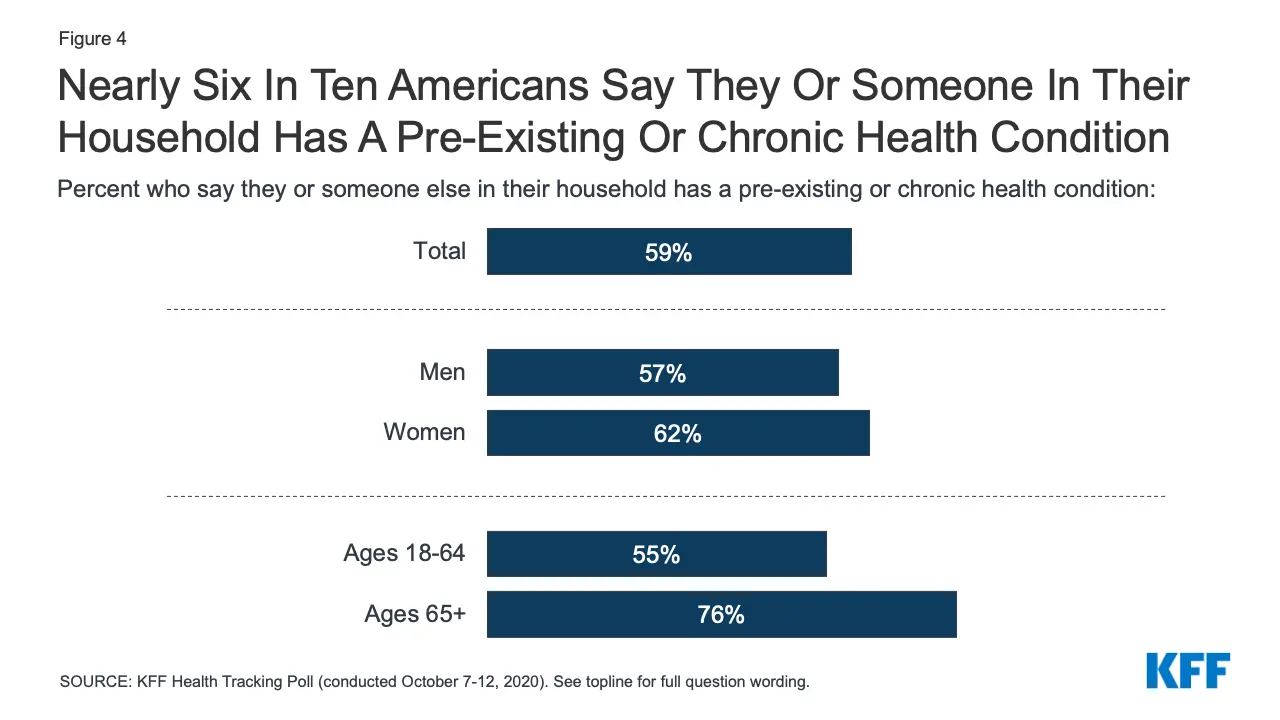
According to the KFF, 59% of people and 79% of people 65 and over, said they, or someone in their household, suffered from a chronic or preexisting condition in 2020.
(Source: KFF)
Conclusion: You Can’t Be Denied Medicare Coverage
You can’t be denied Medicare health insurance coverage. Everyone who qualifies has access to the same Medicare benefits, no matter their current health status or medical history.
The only exception is supplemental cover bought via a Medigap plan.
You have a right to buy a plan at the same price as everyone else during your Medicare Open Enrollment period. But outside this period, insurance providers can turn you down or charge more depending on your condition.