Does Medicare Cover Emergency Room Visits?
Read our guide to find out what Medicare will cover for emergency care and treatment.
Our content follows strict guidelines for editorial accuracy and integrity. Learn about our and how we make money.
If you’re new to Medicare, you’re probably wondering how much coverage the federal health program offers Medicare beneficiaries for emergency medical care and emergency room visits.
While urgent and life-saving medical treatment in the ER can cost a lot of money, you’ll be glad to know that Medicare will cover most of the costs of your visit to the emergency room.
Read our guide to find out what parts of Medicare will cover your treatment and care in the emergency room, and find out what costs you’ll be liable for if you ever need to visit the ER.
What Is Medicare?
The federal Medicare program is a health care program for people over the age of 65, those with certain disabilities, and individuals who suffer from ESRD (End-stage Renal Disease) and ALS (Lou Gehrig’s).
If you are in good health, you qualify for Medicare three months before you turn 65. However, you can enroll at any age after 65.
When you join Medicare, you can either enroll in Original Medicare or Medicare Advantage. Original Medicare consists of Part A and Part B coverage and Medicare Advantage is private health coverage for Part A and B.
Medicare Coverage Explained
There are three parts to Medicare that will cover you for different types of medical expenses.
Part A is hospital coverage and pays for medical costs related to an inpatient hospital stay and hospital treatment.
Part B is outpatient or general medical coverage which covers expenses such as doctors’ visits, routine exams, and outpatient procedures.
Part D is prescription drug coverage for self-administered medication. Original Medicare doesn’t cover this; however, there are private health plans that you can join to pay for these costs.
Medicare Advantage used to be known as Medicare Part C. It covers Part A, Part B, and Part D in some cases.

Source: Pexels
Does Medicare Cover Emergency Room Visits?
Medicare will cover ER visits and trips to the emergency room under either Medicare Part A or Part B.
If you are treated as an outpatient and are up to date with your Part B premiums, you will first need to pay your Medicare Part B deductible to have your treatment covered.
Medicare Part B will cover 80% of the cost of your treatment and you will be liable for the remaining 20% of the cost.
For example, let’s say you are admitted to hospital as an outpatient after a car accident. You receive treatment in the ER and are sent a bill for $12,000. Medicare Part B will pay $9,600 and you will need to pay $2,400.
If you are admitted to hospital as an inpatient, you will be covered for all expenses. However, if you are in hospital for more than 60 days, you will need to pay a coinsurance amount for each day of care.
| Period of Coverage | Coinsurance Amount |
|---|---|
| Days 1 - 60 | $0 per day |
| Days 61 - 90 | $371 per day |
| Days 91 - 120 | $742 per day |
Costs to Keep in Mind
Remember that there are emergency room costs you’ll have to pay regardless of your Medicare coverage when you visit the ER. This includes your monthly premiums, your deductibles, coinsurance amounts, and co-pays.
Besides these costs, there are expenses that aren’t covered by Medicare. For example, ambulance rides aren’t typically covered by Medicare and if you need to be airlifted to the hospital, this can cost you thousands of dollars.

Source: Pexels
Another expense that isn't covered by Medicare is the cost of blood units. The price per pint of blood can range between $150-$350, so if you need four or five blood units, this can end up costing you a lot of money.
If you’re on Original Medicare, it’s a good idea to plan for these expenses and set aside some money to ensure that you can cover these costs if you need them.
You can also look at other insurance coverage options, such as Medicare Supplement Insurance, to help you pay for these uncovered costs.

Source: Pexels
What Is the Medicare Deductible for an Emergency Room Visit?
Deductibles are a fee that you’ll need to pay before you’re covered by your health insurance.
For Medicare Part A you’ll need to pay a deductible of $1,556 in 2022.
For Medicare Part B, you’ll need to pay a deductible of $233 in 2022.
How Much Does an ER Visit Cost?
If you’re ever admitted to the ER, the cost of treatment will depend on the care you require and how long you are in there.
The cost of lifesaving care in the ER can run into thousands of dollars. One thing to note is that you can be treated as an outpatient under Medicare Part B if your injuries aren’t that severe.
However, if you are admitted to hospital, your medical costs will change to inpatient treatment. This means you’ll likely have to pay more than you would as an outpatient, as outpatient treatments have different fee structures.
For example, if you need stitches as an outpatient, you may pay $200. However, if you are an admitted patient, the same procedure may cost you around $400.
If you are admitted to the ER as an outpatient by the emergency department services and at a later point need to be admitted as an inpatient, your outpatient rates will be converted into inpatient rates and you will need to cover the Medicare Part A deductible ($1,556).
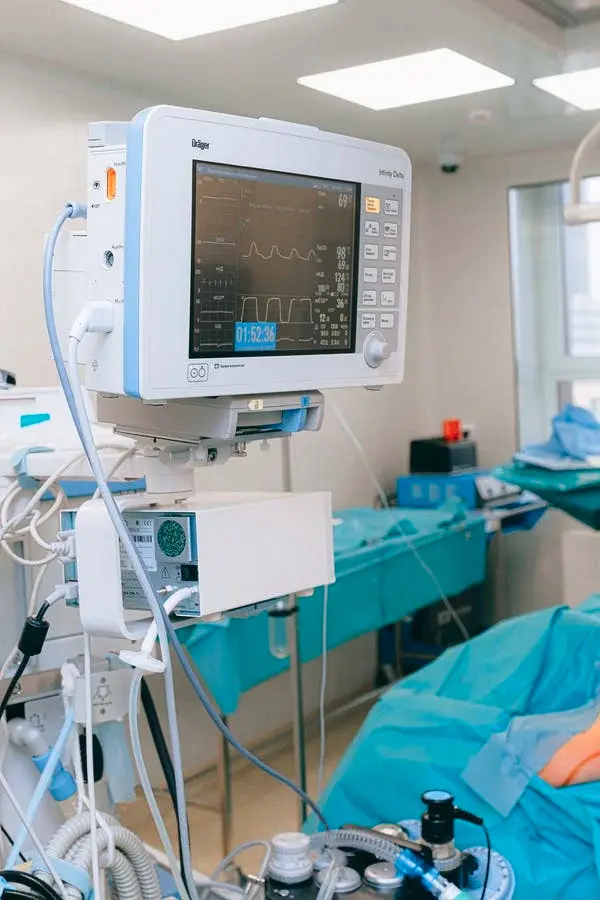
Source: Pexels
Example of ER Costs: Meet George
George is a 68 year-old retiree who experiences chest pain, tingling, and light-headedness while having lunch with his family.
He has Medicare Part A and Part B coverage.
He is rushed to the ER, is diagnosed with a pulmonary embolism, and receives urgent medical care to save his life.
Upon arrival he is given outpatient treatment, but the doctors later decide to admit him to hospital as he needs surgery to clear a blockage in his arteries.
In this case, George’s costs will be converted to Medicare Part A and he will need to pay the Part A deductible to be covered by Medicare.
The Part A deductible for 2022 is $1,556 and once he pays this, he gets up to 60 days of hospital treatment and does not have to pay a coinsurance amount.
If he didn’t have Medicare coverage, he’d have to pay for the entire cost of his treatment as an outpatient and inpatient from his own pocket.
Does Medicare Advantage Cover ER Visits?
Yes, Medicare Advantage Plans are required by law to offer the same or equivalent level of coverage as Original Medicare.
This means that if you are a member of a Medicare Advantage Plan, you’ll get the same care, treatment, and services that a person on Original Medicare receives.
However, most Medicare Advantage Plans usually offer more benefits and perks to their members. Some of these include SilverSneakers, telehealth, and home health care benefits.
In terms of emergency care and emergency room visits, Medicare Advantage Plans offer their members more coverage for added costs not covered by the government Medicare program.
For example, many Medicare Advantage Plans cover the costs of an ambulance ride to and from the hospital, as this trip will be provided by an in-network provider.
They may also not charge their member the 20% coinsurance rate or the per-day Medicare Part A coinsurance rate if they are treated at an in-network hospital or medical facility.
What If I Need ER Treatment While I’m Overseas?
If you’re traveling or on holiday and need to visit the ER, Medicare won’t cover your costs. Our recommendation is to get additional coverage while you’re overseas to ensure that you can get the same level of care as you would in the U.S.

Source: Pixabay
What Other Coverage Options Are There for Emergency Room Visits?
If you’re a member of another type of private health plan, such as Medigap or Part D cover, you may get assistance with the costs of hospital services and treatment in the ER.
Medicare Supplement Insurance
If you have Medicare Supplement Insurance, this can help pay for some of the costs of your emergency room visit or treatment by emergency services.
For example, Medigap Plan F, G, and H all cover the costs of blood transfusions.
Want to find out more about Medicare Supplement Insurance? Read our guides to Medigap cover and Medicare Supplement Insurance Plans.
Medicare Part D (Prescription Drug Coverage)
Medicare Part D may be useful to cover some of the costs of medication after you leave the ER. However, it won’t really help with the costs of treatment while you are in the ER.
If you’d like to learn more about both Medigap and Medicare Part D, be sure to read our guides.
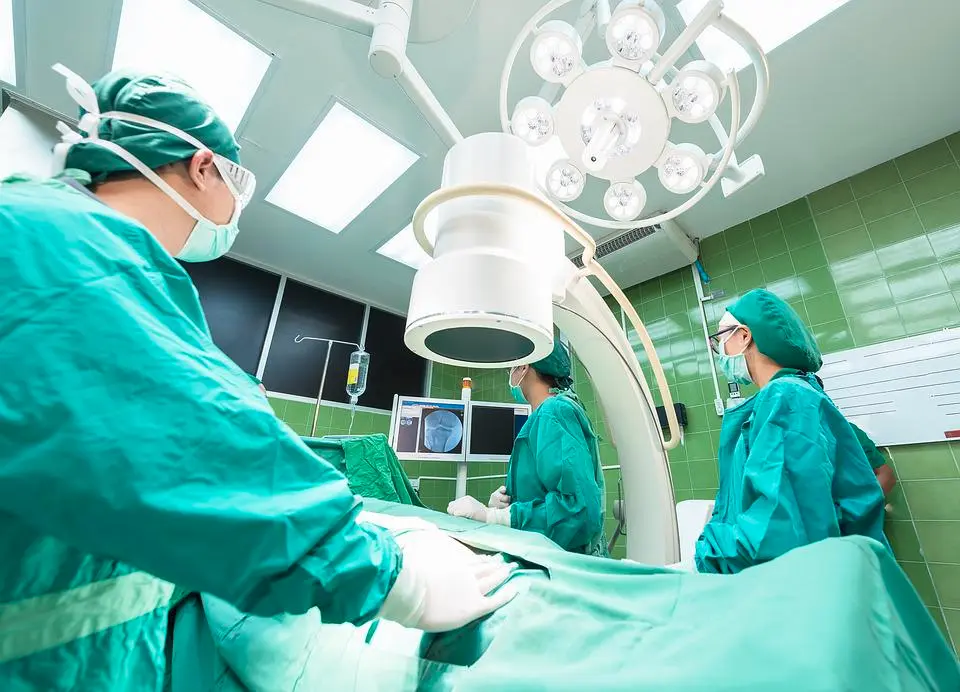
Source: Pixabay
Does Medicare Cover Emergency Room Visits - FAQs
Does Medicare Part A cover emergencies?
Yes, Medicare Part A will cover visits to the ER and medical emergencies if you are admitted to hospital. However, you will need to pay the Part A deductible ($1,556) before you are covered.
What does Medicare Part A pay for?
Medicare Part A covers all inpatient care and treatment on a per-day basis—including emergency room visits. You will be covered for 60 days without having to pay a coinsurance amount. After 60 days, you will need to pay $389 for the next 30 days. After 90 days, you’ll need to pay $778 per day.
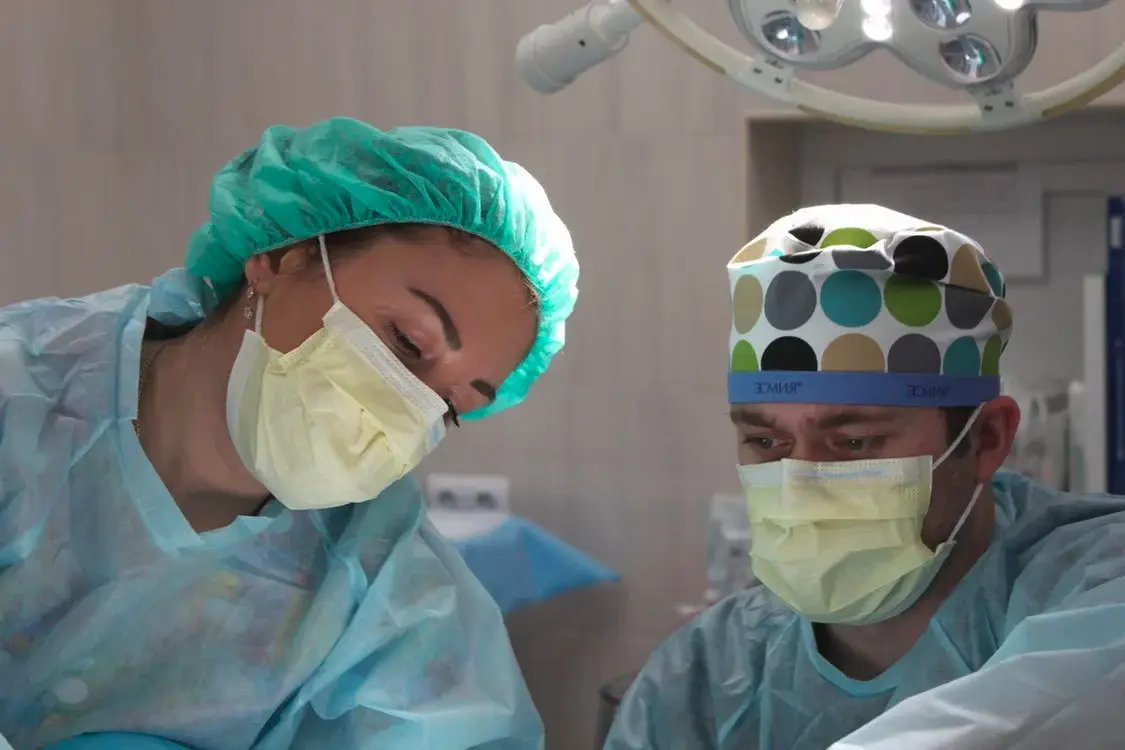
Source: Pexels
Where Can I Learn More about Medicare Coverage and Related Topics?
If you have Original Medicare or a Medicare Advantage Plan, you can rest assured that you’ll be covered in case you need to go to the ER.
However, keep in mind that there are costs that Original Medicare won't cover, such as ambulance services and blood transfusions.
If you’re interested in learning more about Medicare topics such as costs, coverage, and enrollments, be sure to visit our Medicare hub.
If you’d like to speak to someone about your health insurance, speak to one of our Medicare agents to discuss your options and find health coverage in your state.